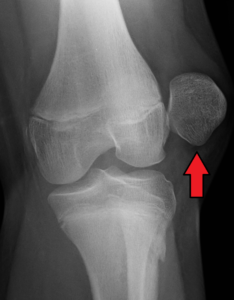
Having a patella dislocation can be a very scary and stressful injury for patients. While any injury can be difficult to deal with, in my experience patella dislocations in particular can be anxiety producing for patients because there is the fear of the unknown – the fear that their patella will dislocate again or the fear that it will happen to their other knee, and how this will affect their ability to continue playing sports or go to school or work. It also conjures up thoughts of needing surgery. The injury can happen from a contact injury, such as colliding with another player during a soccer game, or from a sudden twist or turn. The injury happens very quickly and in some instances the individual may fall to the floor and they may be unable to walk. Their knee may get very big and swollen, and they may end up in the emergency room in order to get their patella relocated. Then they are typically sent home with a brace and instructed to see an orthopedist who specializes in patella injuries like myself. This may be the individual’s first time having such an injury or they may have had recurrent episodes of the patella “shifting” but not dislocating in the past, or this may be the tenth time their patella has dislocated. Regardless of the circumstances, this injury can take a psychological toll on patients and understandably so.
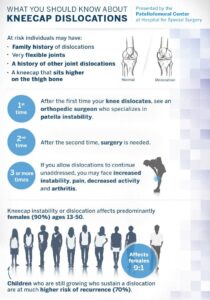
I have dedicated my career to understanding the complexities and intricacies of the patella and there is still a lot we have to learn. I have authored books and done extensive research on the subject of patella instability and pain and have helped develop systematic approaches to the surgical management of these injuries including medial patellofemoral ligament reconstruction (MPFL). I have performed countless surgeries to correct these injuries and have had excellent results and success. Despite all my efforts there is still a lot we don’t know when it comes to selecting the right patients for surgery. For example, a 16-year-old competitive soccer player who comes into my office with her parents after her first patella dislocation during a soccer game. They are devastated by her injury and they may want to have the surgery done as soon as possible to maximize recovery time so as not to miss the following season. The anxiety and tensions are obviously very high, and we have an extensive conversation about patella instability including why the injury likely happened, what the risks are that this will happen again and what I feel is the best approach to managing her injury. Then comes the most difficult part of the conversation, which is that we know that MPFL reconstruction is a safe and effective procedure but what we don’t know for certain yet is whether or not a first-time dislocator should have surgery. The standard of care currently is that non-surgical treatment is the best option for first-time dislocations unless there are other related injuries such as a displaced piece of cartilage in the knee. Explaining to a 16-year-old competitive soccer player and her family that she has a high risk of another dislocation but that she should be treated without surgery is a very difficult conversation to have. This is why I have dedicated years to my current research studies to be able to make a more informed decision with my patients. I am leading a study that aims to answer whether a young first-time dislocator should be treated with surgery called PAPI (Pediatric and Adolescent Patellar Instability). This is a multi-center study in which patients who are selected randomly to either be treated with surgery or without surgery after their first patellar dislocation. Another study that I am leading called JUPITER is a large multi-center patient registry on patellar instability and is the first of its kind in the US. We currently have 28 orthopedic surgeons at 13 centers across the country contributing to JUPITER, and to date have enrolled over 1,200 patients with patellar instability. In the not too distant future, the hope is that the results of these studies will give us a clearer picture of how we should be managing first-time dislocators and patella instability in general, and will allow me to be able to have a more informed conversation with my patients and their families and help to alleviate some of their anxiety and concerns.